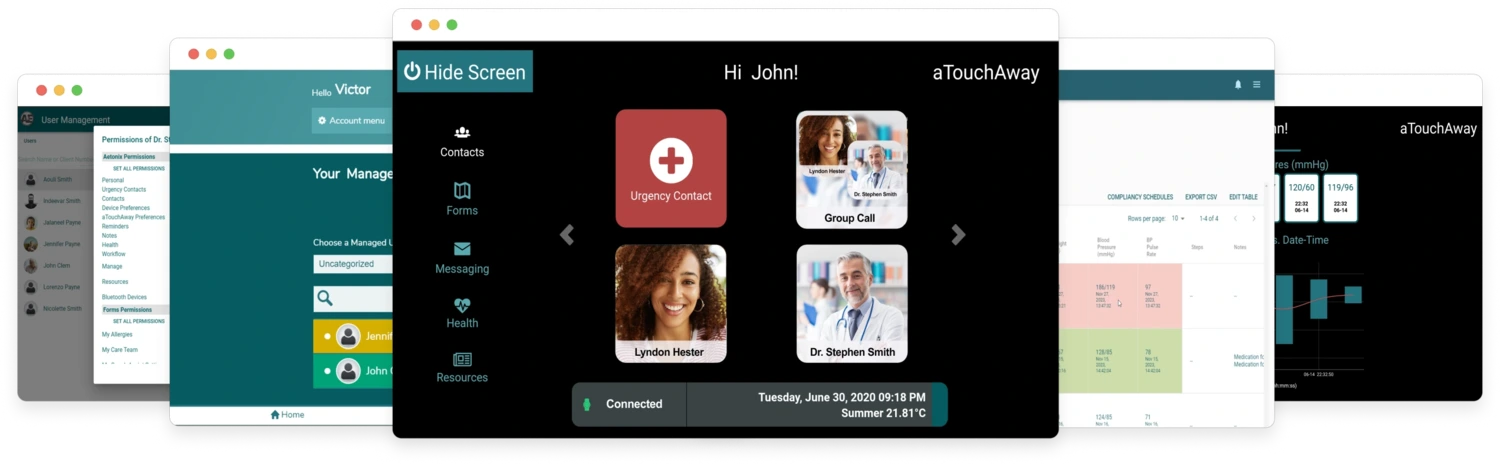
Care Pathways
Explore our innovative Care Pathways designed to revolutionize patient care management.
Our solutions cater to various conditions, providing personalized and effective care plans.

ADVANCED CARE, ENHANCED OUTCOMES
Transforming Patient Care with Advanced Pathways
Discover how our Care Pathways are transforming patient care. These pathways blend medical expertise with technology to deliver personalized care for various conditions, focusing on both treatment and patient empowerment.
Browse Our Active Care Pathways
Chronic Care Pathways
Our Chronic Care Pathways cater to conditions like COPD, Diabetes, and Heart Failure, ensuring continuous and comprehensive support for long-term health management.
Acute Care Pathways
Our Acute Care Pathways offer focused care for urgent medical needs, such as post-surgery and COVID-19 treatments, promoting swift and safe recovery.
Deliver a Seamless, Personalized Patient Journey
Personalized Care Plans
Each pathway is tailored to individual patient needs, ensuring a unique and effective care strategy for one or more conditions while considering procedures and care transitions.

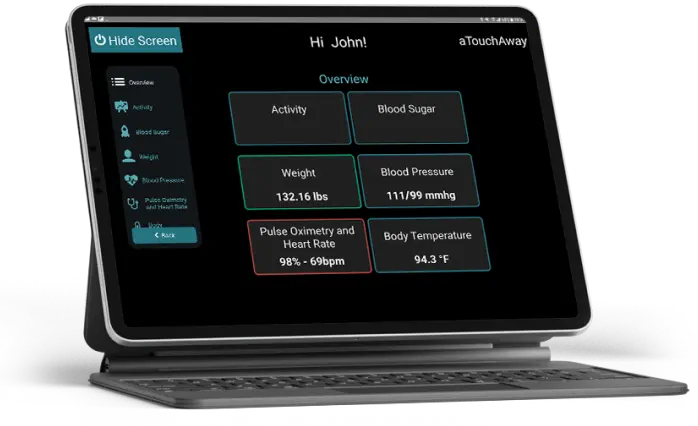
Efficient Care Management
Our pathways streamline the care process through real-time intelligent tracking, making it easier for healthcare providers to manage and monitor patient progress.
Enhanced Patient Outcomes
Focus on improving patient health and reducing hospital readmissions through targeted evidence-based care. This is made possible by the care pathways’ ability to account for the different outcomes that may occur and direct patients to the relevant sequence in the workflow.

Documented Success with aTouchAway®
Real-world evidence demonstrates aTouchAway®’s effectiveness in reducing hospital visits and enhancing patient management.

The Trusted Choice for Enhanced Care.
Join over 250 hospitals and tens of thousands of patients worldwide who rely on aTouchAway®.
Changing Lives Daily.
Using the aTouchAway COPD Care Pathway, we have been able to support our patients at home with required respiratory and oxygen therapy, managing them safely and avoiding unnecessary hospital or clinic visits.
ATouchAway proves to be effective in augmenting patient care while expanding team capacity and saving travel time for our organization.
Miriam Turnbull
VP & GM at ProResp
It’s great. aTouchAway wraps care around the patient at home; patients feel comfort in knowing they have remote access to their care team when they need it. And clinicians can feel confident in knowing they will be alerted when an issue arises, so they can triage when to act to provide safe and efficient care, remotely. The responsive and flexible support team has also been valuable for project implementations and connecting the entire care team.
Colin Catt
Virtual Care Coordinator at Quinte Health Care
With aTouchAway® COPD Care Pathway, I have been able to monitor, guide, and take actions when required for my patients in the community. It has provided me with an additional tool to support a very complex patient population.
Donna Cousineau
Advanced Practice Nurse, Chronic Disease Management, Queensway Carleton Hospital
Ready to Explore aTouchAway®?
Book a demo with one of our service specialists and see how aTouchAway can fit into your practice.